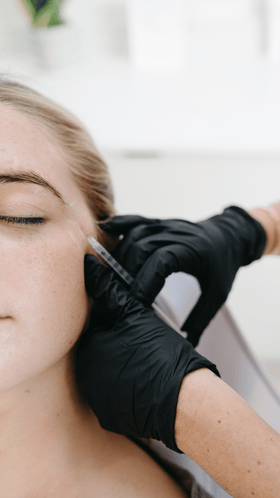
What to expect from a c-section birth

I have teamed up with my good friend and fellow doctor @theobgynmum Brooke who has written about who you can expect to be in the theatre for your section. As a doctor, and having worked in OBGYN I knew what to expect, but as Brooke put’s it, this is all to give you a look behind the proverbial theatre curtain so you are prepared for what happens during an elective section.
Remember this wont be the same for an emergency section where you have laboured but I’ll chat about that at the end. Please bear in mind that this is how it works in the hospital I attend, there may be differences with other hospitals (and obviously coronavirus is affecting everything so there may be significant changes with this also).
The first thing to remember about having a planned section, is you know EXACTLY when you are going to have baby. I’ve always known; never had the surprise, the wonder, the suspense.

Here you meet the midwife that will be looking after you for the day. They will usually go through a full history, full set of vitals etc. If required you will be measured for TEDs stockings and then you wait! Usually your partner / husband would be with you for this stage, but because of coronavirus obviously this isn’t happening at the minute. Now it’s a matter of sitting back and relaxing and waiting to be called for surgery. During this time, you can’t eat or drink. Different hospitals will have different protocols with regards to medications pre-op. In Galway you get a tablet for your stomach. For me, each time I have been on the list pretty early, so I have never had long to wait.
Before going up to the operating theatre you change into your hospital gown (with nothing on underneath!) and usually wear your dressing gown over this. The only other thing you need to bring to theatre is babies first outfit and some blankets. I like to have babies first outfit in a plastic bag all ready to go. In normal times, your husband or partner would accompany you up to theatre. They are usually left outside while you are brought into the anaesthetic room to get ready. Here you meet the midwives and nurses that will be looking after you during the operation. They will check your details and again might go through some vitals making sure everything is ready to go. You will usually meet the anaesthetist at this stage as well, who will insert the cannula ready for theatre. They will go through your medical history again. No-one wants any mistakes made!
Next stage is to be brought into theatre. You will be moved onto the operating table and have the epidural done at this stage. To get this done, you sit on the edge of the bed, legs on a step and bent over slightly (so there is a slight curve in spine) with a pillow tucked in front of you. The anaesthetist will talk you through every step so you know what’s happening. Once the epidural is in and meds have been given you will start to feel them working. A heaviness / hot feeling will move down your legs and you will lie back on the table.
There will be lots of people around you in theatre at this stage and they will start getting everything ready. You wont be able to feel your legs after a couple of minutes and usually right up to your nipples. The theatre nurse will be setting everything up and putting up a drape in front of you so that you can’t see what’s happening. Your arms are usually brought out at right angles to your body, and hooked up to BP monitors etc. While this is all happening they will usually be placing a catheter into your bladder and getting you all cleaned for surgery. All of the goes by really quickly and honestly before you know it they are operating. The next thing you will be told is that baby is coming out. During non-coved times, husband / or partner would usually be brought in now to see baby being born. Time from knife-to-skin to baby being born is pretty quick, around 5-10 minutes if it is your first baby but slightly longer if you have had operations before. Its the stuff afterwards that takes much longer! The whole operation (without any issues) takes 45 minutes - 1 hour.
While the drape is up in front of you during the operation, they will pull the drape down and show you baby once they are out! If possible they will do delayed cord clamping if you wish. Each hospital is different with regards to what happens next. In Galway, the midwife looking after baby takes them to check over everything. 10 fingers,10 toes; umbilical cord clamping, weigh baby etc. I’ve always wanted skin-to-skin so once this is done they are brought in and put on your chest for as long as possible.
On Romy’s birth, because Ross wasn’t allowed into theatre I sent Romy out to him for some cuddles (or skin to skin if dad wants) before I got out of theatre. The other thing to remember is that sometimes you can feel a bit sick during the operation because blood pressure drops etc with morphine and you might not want to have baby on your chest for the whole time.
After this it is a case of stitching you up. If there aren’t any issues, they can be done really quickly and you can be out feeding baby in no time. I think I was out within 25 minutes with Harper, but it took a bit longer with Indie. Romy again was super quick.

Most women will stay 2-3 nights in hospital after an uncomplicated C section and that will depend on how your recovery goes.
To chat just a little bit about emergency sections. Obviously all of mine have been planned, and as I mentioned at the start emergency sections are very different to electives. Usually they happen because labour isn’t progressing as hoped, or else because of an emergency with baby. Emergency sections are categorised by how quickly they need to happen from the time they are called. So for example if baby is in distress then they are a category 1 section and usually this means that baby needs to be delivered ASAP (within 30 mins). Category 2 sections are usually within the hour - if it’s due to failure to progress for example. Category 3 means the baby needs to be born early, but with no immediate risk to mother or baby and category 4 are elective sections. Unfortunately in an emergency there may not be time to give you an epidural and so sometimes a general anaesthetic will be used (though this is rare).
Recovery can obviously be much harder after an emergency as you may have laboured or been induced prior to then undergoing major surgery so its good to be aware of this.
Its important to remember as well that there are risk to having a section (some of which can occur with a vagianl birth as well obviously). But I want to make sure you have the whole picture.
The main risks include:
- infection of the wound (common) – causing redness, swelling, increasing pain and discharge from the wound
- infection of the womb lining (common) – symptoms include a fever, tummy pain, abnormal vaginal discharge and heavy vaginal bleeding
- excessive bleeding (uncommon) – this may require a blood transfusion in severe cases, or possibly further surgery to stop the bleeding
- deep vein thrombosis (DVT) (rare) – a blood clot in your leg, which can cause pain and swelling, and could be very dangerous if it travels to the lungs (pulmonary embolism)
- damage to your bladder or the tubes that connect the kidneys and bladder (rare) – this may require further surgery

So who exactly are all the people in the operating theatre?

Who is present in theatre
One thing that many women, and their partners, are often quite surprised by, is how many people are often present in the theatre. It can make you feel quite overwhelmed. Therefore it can be really helpful to understand who you could expect to be there, and remember that everyone there has a role to play in looking after you and your baby:
Obstetricians
These are the surgeons who perform the C section. We need 2 people (at least), and they are usually a junior and senior doctor who work together to do the operation. There is usually a third obstetrician, the consultant, who may be present in theatre, elsewhere on the labour ward or available by phone to call if there are any complications.
Scrub nurse
These nurses are specially trained to assist in operations by scrubbing in, and handling all the instruments, ensuring the surgeons are presented with the tools they need at the right time.
Anaesthetist
This is a doctor who is specially trained at providing pain relief, as well as putting you to sleep if needed. They sit near your head, closely monitoring all your vital signs and can reassure you and talk to you throughout.
Operating department Practitioners (ODP)
These are the assistants to the anaesthetist and prepare the environment and equipment they need
Midwife
Even if your birth is by operation, a midwife is there to support you for birth, check over your baby and help you with feeding and your postnatal recovery
Paediatrician
In most hospitals the baby doctors will be present for any emergency C sections, and some elective ones to check the baby at birth and assist if needed.
Healthcare Assistant
Vital team members for moving patients, cleaning and assisting other staff.
Other staff members may be called on including:
Ok, I think that is all I can say about sections. Have you had a section? How did it go? Let me know over on the instagram post and don’t forget to give it some love if you found it useful.
Thanks again,
Dr Laura x